Imagine stepping into the sun, expecting a warm glow on your skin, and instead, you start itching, or even worse, developing a rash.
Welcome to the world of sun allergies – a bit less common, but very real and quite a bummer, to be honest.
That’s right — you can be allergic to the sun!
Not everyone can frolic in the sunshine with glistening skin, some of us have to battle the evil sun’s rays a bit harder.
Let’s shed some light on this, shall we?
What’s a Sun Allergy Anyway?
A sun allergy is quite different from a sun burn — while a sun burn is basically a skin injury from excessive UV radiation, a sun allergy, also known as photodermatosis, is a more complex reaction involving the immune system responding to sunlight.
Unlike sunburn, a sun allergy isn’t caused by overexposure to the sun per se. Instead, it’s an overreaction by the body’s immune system to sunlight, triggering an allergic response.
Types of Sun Allergies: Meet the Unwanted Guests
To be the ultimate sun warrior, you need to know your enemy. So, let’s get acquainted with these sun allergy types, shall we?
1. Polymorphous Light Eruption (PMLE)
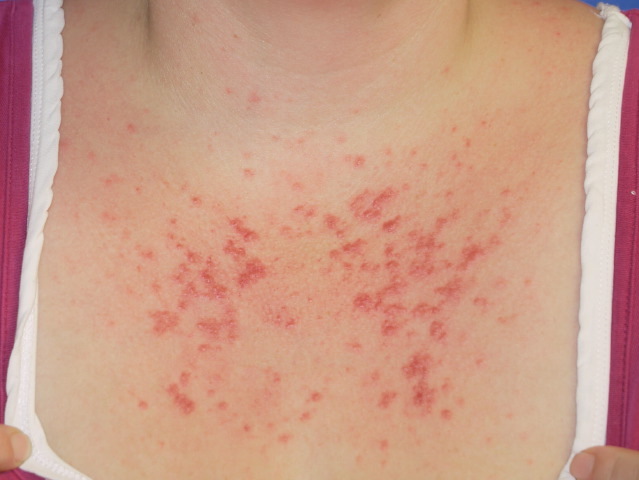
Polymorphous Light Eruption, commonly referred to as PMLE, is the most common sun allergy out there. In fact, it’s estimated that 10-15% of the US population are affected by PMLE, although it may even be higher due to underreporting.
PMLE frequently makes its appearance in spring or early summer, often disrupting your plans for outdoor leisure (so rude).
The primary symptoms are an uncomfortable, itchy rash that may present as red, raised patches or even as small bumps. The rash usually occurs on areas of the body that have recently been exposed to the sun— in particular, areas that don’t see much sun during the colder seasons, including the neckline and the lower legs.
In severe cases of polymorphous light eruption, people may also experience flu-like symptoms such as headaches and nausea.
2. Actinic Prurigo
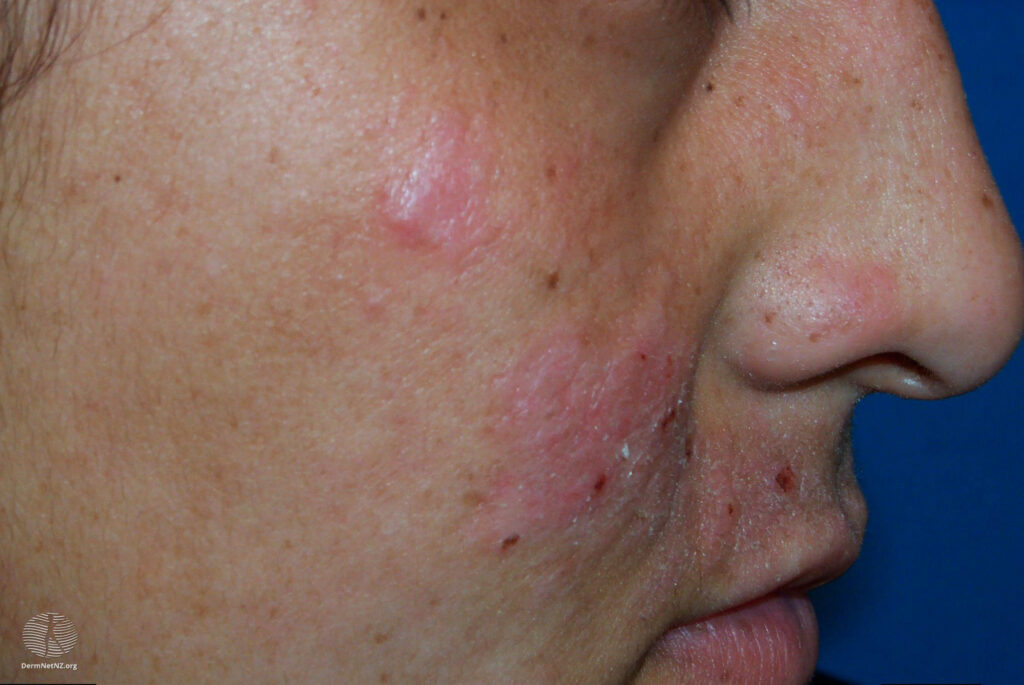
Actinic Prurigo, unlike PMLE, isn’t merely a seasonal phenomenon; it can persist throughout the year, rearing its mean ol’ head at any time.
This form of sun allergy typically causes itchy, scaly patches, often manifesting on more exposed areas of the skin, such as on the face, arms, and hands.
Occasionally, the patches may develop into persistent sores or wounds – yikes!
It’s generally more common in individuals with Native American ancestry, and can be quite challenging to manage, requiring ongoing treatment and vigilant sun protection.
3. Solar Urticaria

Solar Urticaria is a fairly rare form of sun allergy, and it isn’t here to mess around – it can push your body to produce hives within mere minutes of sun exposure.
The symptoms include redness, itchiness and the inflammation of the skin into raised welts – much like those seen with a typical allergic reaction. The hives can vary in size and are usually short-lived, disappearing within hours as long as further sun exposure is avoided.
In severe instances, solar urticaria might lead to breathing difficulties, headaches, and nausea.
4. Chronic Actinic Dermatitis (CAD)

Chronic Actinic Dermatitis (CAD) is another less-common but frustrating chronic rash that can be induced by exposure to the sun. Not only that, it can also be triggered by certain artificial lights – that’s right, you’re glowing TV screen or smartphone can be part of the problem as well.
The symptoms of CAD include dry, scaly patches on the skin and itchiness, which can become more severe with added exposure to light sources. The rash primarily affects sun-exposed skin, but may also spread to other areas too.
CAD typically demands stringent sun-protection measures (we’re talking sunscreen, sun hats, shawls, the whole nine yards) and in some cases, intervention with steroidal creams or systemic medication to manage effectively.
While these conditions may seem daunting, remember that each can be addressed and managed with a bit of elbow grease and a good attitude.
If you think you’re suffering from a sun allergy, it’s crucial to get the assessment of a dermatologist. They’ll help clarify your specific condition, and then together, you can formulate the best plan of action.
Sun Allergy Symptoms: Signs You May Be Allergic to the Sun
Wondering if you have a sun allergy? Let’s review the most common sun allergy symptoms:
- Redness or Rash: Sun allergies often present with redness or a rash on the sun-exposed skin. The rash may appear as tiny blisters or slightly raised patches of skin.
- Itching and Tingling: The skin areas affected by the allergy can feel itchy or have a tingling sensation, which can range from mild to intense.
- Swelling and Bumps: Some people experience an allergic reaction that causes swelling and bumps on the skin.
- Hives: Particularly in conditions like Solar Urticaria, you might see hives or welts form on the skin following UV exposure.
- Scaling or Bleeding: In certain forms of sun allergy, like Actinic Prurigo, the patches can turn scaly or even bleed.
- Pain or Discomfort: Affected areas may feel sore or uncomfortable, especially when touched or exposed again to sunlight.
- Headaches and Fever: In severe cases, people can experience flu-like symptoms like headaches or fever.
Remember, these symptoms can vary from person to person, both in intensity and type. If you experience any of them consistently after sun exposure, be sure to reach out to a dermatologist for an evaluation.
Sunburn vs Sun Allergy: What’s the Difference?
A sunburn features red skin that’s hot and sensitive to the touch, and that might blister over time. Sunburns often don’t become obvious until several hours after sun exposure — or even the next day!
Sun allergy reactions, on the other hand, can occur within minutes. They usually appear as an itchy or burning rash.
Risk Factors: What Causes Sun Allergies?
Let’s delve into the key risk factors that can elevate your chances of developing sun allergies
Sun allergies could be due to:
- Genetic Predisposition. Some sun allergies have a hereditary component. If sun allergy runs in your family, you might be more likely to experience it too.
- Certain Medications. Believe it or not, certain medications can make your skin more susceptible to sun allergies. These can include antibiotics, some types of pain relievers, and certain antidepressants. These photosensitizing medications absorb UV light and then release it into the skin, causing a reaction. Always check medication labels for sun sensitivity warnings or discuss with your healthcare provider.
- Specific Skin Products. Certain skin products, particularly those containing fragrances, may have ingredients that trigger a phototoxic reaction when exposed to UV light, making your skin more susceptible to sun damage. Be sure to scrutinize the labels for potential photosensitizing ingredients like bergamot, lime, cumin, ginger, and orange.
- Autoimmune Disorders. Certain autoimmune disorders, like lupus, can make individuals more susceptible to sun allergies. This can be true for any ongoing infection as well. We’d recommend those folks opt for mineral sunscreens that put up a tough outer barrier on your skin to keep sunlight out (check out our list of the best sunscreens for lupus for some suggestions).
- Exposure after a Period of Limited Sunlight. Some people may experience a sun allergic reaction during the early days of summer or during a tropical vacation, especially if their skin has not been exposed to sun for a while.
- Age. Some types of sun allergies (like Actinic Prurigo) often begin in childhood or adolescence.
- Skin Type. Those with fair skin or those low on the Fitzpatrick skin type scale may be more likely to develop a sun allergy, though it can occur in any skin type.
- Environmental Factors. Environmental conditions can play a significant role in sun allergies. Intense sunlight in summer or at high altitudes, combined with excessive heat, can increase your chances of a reaction, especially if your skin is not accustomed to such exposure.
How Do Doctors Asses a Sun Allergy?
Thinking you might be dealing with more than a typical sunburn? Here’s a more comprehensive look into the process of how medical professionals determine whether or not you have an allergy to the sun’s bright rays:
1. Medical History: The first detective in uncovering whether you have a sun allergy might just be your own medical history. Your healthcare provider is likely to initiate the process by starting a dialogue on your symptoms, their severity, frequency, and potential triggers. Recurrent symptoms coinciding with sun exposure could be a telltale sign!
2. Physical Examination: Sometimes, your skin may be holding all the answers. Through a detailed physical examination, your doctor can scrutinize any skin reactions or changes that might provide clues towards a sun allergy rather than standard sunburn.
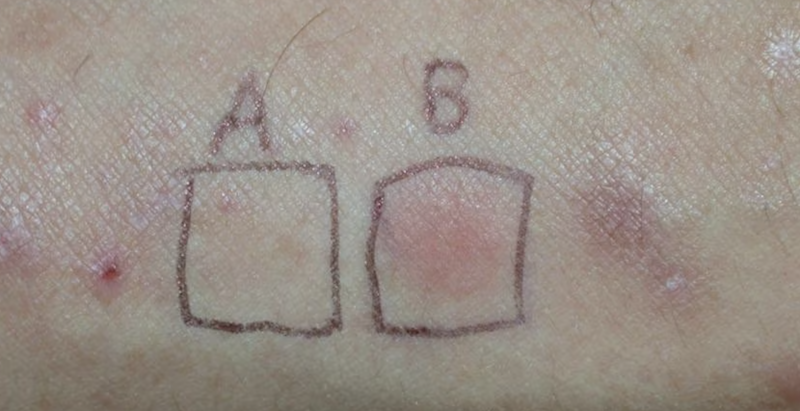
3. Skin Tests: Skin tests serve up important data to diagnose the specific type of your sun allergy. These tests typically involve the application of photosensitizing substances to a small skin surface, followed by controlled UV light exposure, all in an effort to provoke a reaction helping identify the exact nature of the allergy.
4. Blood Tests: These can operate as the undercover agents in this detective tale, helping to rule out other conditions that could mimic sun allergies. By examining the count and condition of certain cells, healthcare providers can validate or rule out alternatives like lupus or dermatitis.
5. Phototests: The phototest, a more specific type of skin test, involves exposure of different skin portions to measured dosages of UVA and UVB light. If sunlight is the culprit behind your skin woes, this test would most likely bring about similar reactions to the ones you regularly experience following sun exposure.
Each method brings its own set of benefits and limitations, so your healthcare provider will weave together a diagnostic plan that’s the best fit for you.
When To Contact Your Doctor
If you find yourself exhibiting signs of a sun allergy— persistent itching, redness, swelling or discomfort following sun exposure— do not hesitate to consult a healthcare professional. Remember, in the realm of health, it’s always better to err on the side of caution!
Sun Allergy Treatments & Prevention
Finding out you have a sun allergy may be a little daunting, but fear not! There’s an arsenal of fighting strategies at your disposal to overcome this hurdle:
- Sunscreen: Your Shield and Protector. The first line of defense against a sun allergy is solid sunscreen protection. Make broad-spectrum sunscreens with a high SPF rating your silent guardians. These sunscreens offer protection against both UVA and UVB rays, reducing the potential for triggering allergic reactions — we’d especially recommend mineral sunscreens for the skin sensitive.
- Clothing: Your Stylish Barrier. A picture-perfect mix of fashion and function, Ultra Violet Protection Factor (UPF) clothing can serve as an additional safeguard from harmful sun rays. From UPF shirts to wide-brimmed hats, infusing these items into your wardrobe can mean extra skin safety.
- Medication: Your Secret Weapon. Depending on the nature of your sun allergy, your healthcare provider might arm you with specific medications, such as antihistamines for suppressing allergy symptoms or corticosteroid creams for reducing inflammation and discomfort.
- Phototherapy: Light vs. Light. Yes, it sounds a bit like fighting fire with fire, but phototherapy—controlled exposure to certain kinds of light—can help your skin grow resilient over time. The light doses begin low and gradually increase, with the aim being to accustom your skin to sunlight without triggering an allergic reaction.
- Lifestyle Changes: The Key to Victory. Small daily adjustments can add a powerful punch to your fight against sun allergies. Seeking shade during high-sun-intensity hours (10 a.m to 4 p.m), hydrating adequately to maintain skin health, and regularly donning sunglasses to protect the delicate skin around your eyes can make a substantial difference.
Remember, living with a sun allergy doesn’t mean living in fear of the sun. With proper measures in place and efficient management, you can continue to enjoy sunny days—just with a little more caution and a lot more sunscreen!
FAQ About Sun Allergies
How can you tell the difference between a sun allergy and sunburn?
Sun allergy and sunburn both manifest after sun exposure but there are key differences. A sunburn usually presents as painful, reddened skin that can blister or peel over time, affecting any sun-exposed skin regardless of prior exposure. Sun allergy reactions often appear as an itchy, red rash (often immediately following sun exposure or soon after) and usually occur on skin that has been covered during cooler months (think: neck, back of hands, lower legs).
How do I prevent sun allergies from affecting my eyes?
Eyewear with UV-protective lenses is your first line of defense. Wearing a wide-brimmed hat can also provide additional protection. Avoid direct sun exposure in peak intensity hours if possible, and seek shade whenever you can.
What’s the best way to cope with the emotional and social impact of having a sun allergy?
Dealing with a sun allergy can be emotionally challenging. Learning to manage your condition can increase control and decrease anxiety. Reach out to support groups, physical or online, where people share their experiences and coping strategies. You’re not alone in this!
How to find a dermatologist who specializes in sun allergies?
You can start by asking your primary care provider for a referral. You could also check with local hospitals or medical schools, or visit the website of the American Academy of Dermatology, which has a directory of dermatologists.
How do I calm a sun allergy reaction?
At the first sign of reaction, move out of the sun immediately and cover up your skin. A cool shower or cool compresses can help soothe the skin. Over-the-counter creams that contain cortisone can alleviate itching and inflammation. If symptoms persist, seek medical attention.
Can you use an antihistamine for a sun allergy?
Yes, antihistamines can be used to alleviate some of the symptoms of a sun allergy such as itching and swelling. However, they should be taken as directed by a healthcare professional, who can guide you to the best treatment based on your individual symptoms and medical history.

